Hydrochlorothiazide rash — causes, symptoms, treatment and prevention
Table of Contents
- What is hydrochlorothiazide rash?
- How HCTZ works and why it can cause rash
- Types of rashes linked to hydrochlorothiazide
- Symptoms and signs to watch for
- Diagnosis and differential diagnoses
- Risk factors — who is more likely
- Management and treatment options
- Prevention and alternatives
- When to seek emergency care
- Patient advice, FAQs, and follow-up
What is hydrochlorothiazide rash?
Users exploring hypertension treatment solutions sometimes choose to buy hydrochlorothiazide without prescription online while comparing delivery conditions and pharmacy availability.
Hydrochlorothiazide rash refers to any cutaneous reaction linked to the commonly prescribed thiazide diuretic hydrochlorothiazide (HCTZ). While HCTZ is effective for treating hypertension and edema, a subset of people experience skin reactions that vary in appearance and severity. These can be benign, like minor itchy bumps, or serious, like Stevens-Johnson syndrome (SJS) or toxic epidermal necrolysis (TEN). Recognizing the difference early is crucial because treatment ranges from stopping the drug and using topical creams to urgent hospitalization for life-threatening reactions.
How HCTZ works and why it can cause rash
Hydrochlorothiazide lowers blood pressure by increasing the kidney's excretion of sodium and water. Its pharmacologic action is unrelated to the skin, so why do rashes occur? Mechanisms include immune-mediated hypersensitivity, photosensitivity reactions where UV exposure alters the drug in the skin, and direct non-immune irritant effects. In immune-mediated cases, the body recognizes HCTZ or its metabolites as foreign, triggering T-cell responses that cause inflammation and skin cell damage. Photosensitivity stems from HCTZ absorbing UV light and producing reactive oxygen species that damage skin cells and provoke dermatitis.
Types of rashes linked to hydrochlorothiazide
Several rash types are associated with hydrochlorothiazide, each with different timing, appearance, and severity. Common categories include:
- Morbilliform (measles-like) eruptions — diffuse red macules and papules.
- Urticaria — itchy, transient wheals often linked to allergic reactions.
- Photosensitivity — sun-exposed areas show exaggerated sunburn or pigmented patches.
- Fixed drug eruptions — recurrent localized dark patches after re-exposure.
- Severe cutaneous adverse reactions (SCARs) — SJS/TEN and drug reaction with eosinophilia and systemic symptoms (DRESS).
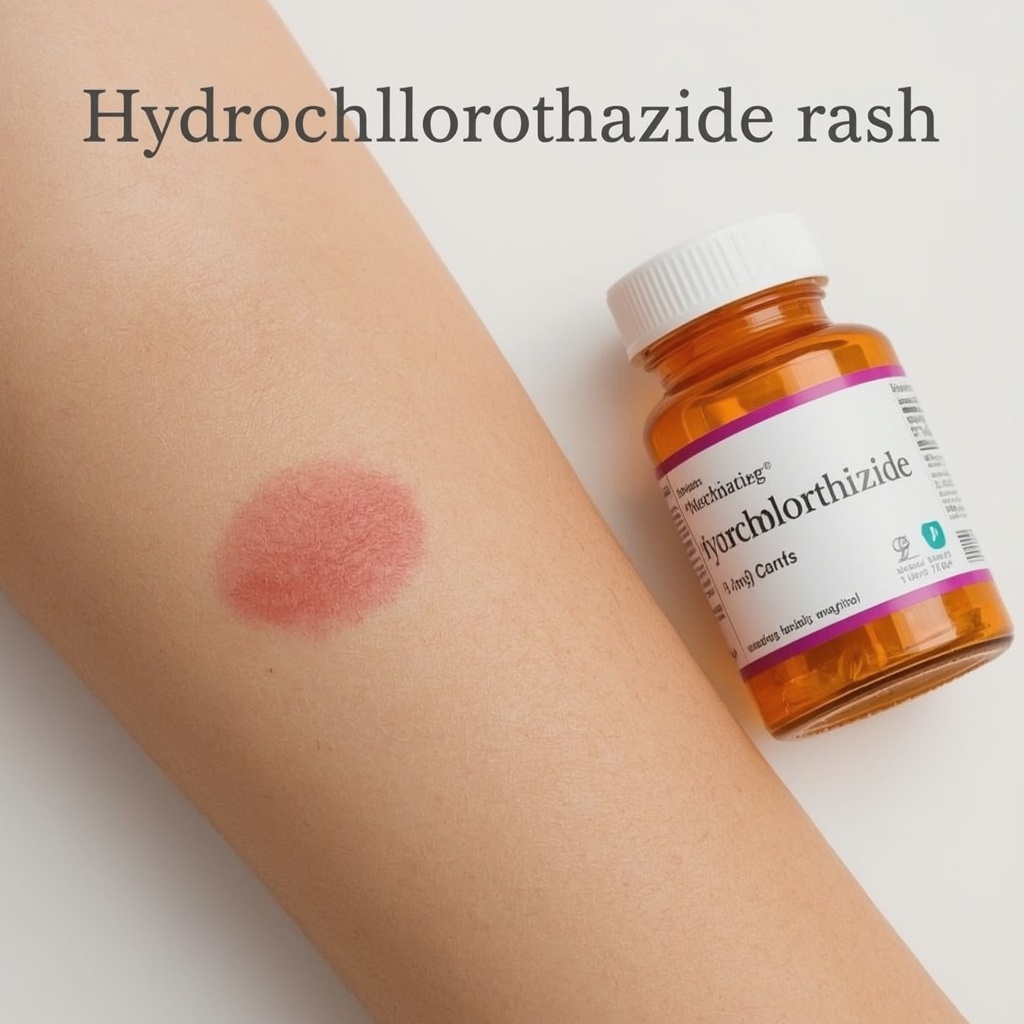
Onset varies: some rashes appear within days, others after weeks or months. SCARs are less common but require immediate attention; they can begin as flu-like symptoms followed by rapidly progressing blistering and mucosal involvement.
Symptoms and signs to watch for
Knowing the red flags of a hydrochlorothiazide rash helps patients and clinicians act quickly. Mild reactions include localized redness, itching, and small bumps. Concerning features include rapidly spreading rash, blisters, skin peeling, mucous membrane sores, fever, swollen lymph nodes, and systemic symptoms like difficulty breathing or low blood pressure. Photosensitivity typically presents as an exaggerated sunburn pattern with itching or hyperpigmentation on sun-exposed areas.
Key symptoms to watch for:
- Widespread redness or blistering
- Mucosal sores (mouth, eyes, genitals)
- High fever or malaise preceding the rash
- Shortness of breath or facial swelling (possible anaphylaxis)
- Persistent or worsening rash after stopping other common causes
Diagnosis and differential diagnoses
Diagnosing hydrochlorothiazide rash starts with history and physical exam: timing of drug initiation, rash appearance, distribution, and associated symptoms. Important differential diagnoses include viral exanthems, contact dermatitis, autoimmune blistering diseases, and rashes from other medications (ACE inhibitors, NSAIDs, antibiotics). Laboratory tests such as CBC (for eosinophilia), liver and kidney panels, and occasionally skin biopsy or patch testing can clarify the cause. For suspected SJS/TEN, clinical evaluation is urgent and often supplemented by dermatology consultation and biopsy to confirm epidermal necrosis.
Risk factors — who is more likely
Certain factors increase the chance of developing a hydrochlorothiazide rash. Age (older adults), cumulative sun exposure, female sex (some studies suggest higher reporting), polypharmacy, and previous drug allergies raise risk. Genetic predisposition affecting immune response or drug metabolism may also play a role. Patients with autoimmune disease or those taking other photosensitizing medications face higher likelihood of photosensitive reactions.
| Risk Factor | How it increases risk |
|---|---|
| Age (older adults) | Altered drug metabolism and immune response |
| Sun exposure | Triggers photosensitivity reactions with HCTZ |
| Polypharmacy | Higher chance of drug interactions and cumulative photosensitizers |
| Prior drug allergies | Increased immune sensitization to new drugs |
Management and treatment options
Treatment depends on severity. For mild hydrochlorothiazide rash, the first step is stopping HCTZ and using supportive care: topical corticosteroids, emollients, and oral antihistamines for itching. Moderate reactions may need short oral steroid courses. Severe reactions like SJS/TEN or DRESS require hospitalization, often in a burn unit or ICU, intravenous fluids, wound care, systemic immunosuppression, and multidisciplinary management.
Practical steps for mild-to-moderate reactions:
- Stop hydrochlorothiazide immediately and inform your prescriber.
- Use oral antihistamines (cetirizine, diphenhydramine) for itch relief.
- Apply medium-potency topical steroid to inflamed areas.
- Protect skin from sun exposure and avoid heat and harsh soaps.
| Severity | Treatment | Follow-up |
|---|---|---|
| Mild (localized itching/redness) | Stop HCTZ, topical steroids, oral antihistamines | Primary care follow-up within 1 week |
| Moderate (widespread rash, systemic symptoms) | Oral corticosteroids, dermatology consult | Close outpatient monitoring or short admission |
| Severe (SJS/TEN, DRESS) | Hospitalize, IV fluids, specialized wound care, systemic therapy | Long-term follow-up for scarring and sequelae |
Prevention and alternatives
Preventing hydrochlorothiazide rash starts with clinician awareness and patient education. If you have a history of photosensitivity or prior drug rashes, discuss alternatives with your provider. Protective measures—broad-spectrum sunscreen, sun-protective clothing, and avoiding peak UV hours—reduce photosensitivity risk. If HCTZ is suspected as the culprit, clinicians may switch to alternative antihypertensives or diuretics such as indapamide, spironolactone, or a low-dose ACE inhibitor or ARB, depending on the clinical context.
Comparison of common diuretic options and rash risk:
| Medication | Rash/photosensitivity risk | Considerations |
|---|---|---|
| Hydrochlorothiazide (HCTZ) | Higher photosensitivity and allergic rash risk | Effective for HTN; monitor for skin reactions |
| Indapamide | Lower reported photosensitivity | Similar efficacy to HCTZ in many patients |
| Spironolactone | Low photosensitivity; other side effects (gynecomastia) | Useful for resistant HTN, heart failure |
When to seek emergency care
Some hydrochlorothiazide rashes are medical emergencies. Seek immediate care or call emergency services if you experience rapidly spreading blisters, large areas of skin peeling, painful red eyes or mouth sores, difficulty breathing, facial swelling, high fever, or signs of sepsis (fast heart rate, dizziness, fainting). Early recognition of SJS/TEN and immediate cessation of the offending drug improve outcomes. If you suspect anaphylaxis (wheezing, throat tightness, hypotension), use epinephrine if available and emergency services should be called without delay.
Patient advice, FAQs, and follow-up
Patients often ask whether they can restart hydrochlorothiazide after a rash. The general rule: do not restart if the rash was moderate to severe, atypical, or involved mucosa. For mild, clearly non-immune reactions, clinicians may consider rechallenge rarely and under supervision, but alternatives are usually safer. Allergy testing for HCTZ is not routinely available; patch testing or lymphocyte transformation tests are sometimes used in specialized centers.
Quick FAQ:
- Can HCTZ cause sunburn? Yes — photosensitivity can mimic severe sunburn.
- Is rash dose-dependent? Not reliably — reactions are often immune-mediated rather than dose-related.
- Do topical steroids help? They can reduce inflammation for mild reactions but won’t stop severe SCARs.
Follow-up after any drug rash should include documentation in medical records, allergy alerts in patient charts, and discussion of alternative therapies. Report severe adverse reactions to your health authority or FDA MedWatch to contribute to drug safety data.
FAQ
What is a hydrochlorothiazide rash?
A hydrochlorothiazide rash is a skin reaction triggered by the diuretic hydrochlorothiazide (HCTZ). It can range from mild red bumps or hives to more severe blistering or widespread rashes. Causes include allergic immune responses and photosensitivity; presentation and severity vary between individuals.
How common is an HCTZ rash?
Mild cutaneous reactions to HCTZ are relatively uncommon but not rare. Severe reactions like Stevens-Johnson syndrome are very rare. Incidence depends on population, dose, and individual susceptibility; most people taking HCTZ do not develop a rash.
What does a hydrochlorothiazide rash look like?
Appearance varies: small red macules or papules, widespread erythema, urticaria (hives), or in rare severe cases blisters and targetoid lesions. Photosensitivity rashes typically appear on sun-exposed areas. Distribution, associated symptoms, and timing help characterize the rash.
When does an HCTZ rash typically appear after starting the drug?
Onset can be within hours to days for immediate allergic reactions, or several days to weeks for delayed hypersensitivity. Photosensitivity reactions may appear after sun exposure while taking the medication. Late-onset severe reactions can occur weeks after starting.
What causes a rash from hydrochlorothiazide?
Rashes from HCTZ result from immune-mediated hypersensitivity, direct phototoxic/photoallergic effects, or idiosyncratic reactions. The thiazide chemical structure can promote photosensitivity and, in some people, trigger a drug allergy with immune activation in the skin.
Who is at higher risk for developing an HCTZ rash?
Risk factors include prior drug allergies, history of photosensitivity, fair skin, high cumulative sun exposure while taking HCTZ, concurrent medications that increase photosensitivity, older age, and certain genetic or immune predispositions. A prior severe sulfa antibiotic reaction warrants caution.
Is hydrochlorothiazide a sulfa drug and does that matter for rash risk?
HCTZ has a sulfonamide moiety but is not the same as sulfonamide antibiotics. Cross-reactivity is possible but not guaranteed. People with a history of severe immediate reactions to sulfa antibiotics should discuss alternatives and allergy testing with a clinician before using HCTZ.
Can hydrochlorothiazide cause severe reactions like Stevens-Johnson syndrome or TEN?
Yes, although very rare, HCTZ has been reported to trigger severe cutaneous adverse reactions such as Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN). These conditions are medical emergencies—look for widespread blistering, mucosal involvement, fever, and systemic illness.
How is an HCTZ-related rash diagnosed?
Diagnosis is primarily clinical: history of HCTZ exposure, rash timing, appearance, and symptom pattern. Blood tests, skin biopsy, or allergy testing may be used when the diagnosis is unclear or if a severe reaction is suspected. Dermatology or allergy consultation helps with complex cases.
What is the first-line treatment for a hydrochlorothiazide rash?
Mild cases often improve after stopping HCTZ and using supportive care: topical corticosteroids, oral antihistamines for itch, and skin emollients. Moderate-to-severe reactions may require systemic corticosteroids, hospital monitoring, and specialist care. Always consult your prescriber before stopping any medication.
Can I keep taking hydrochlorothiazide if the rash is mild?
You should contact your prescriber before continuing. Some mild rashes may be monitored, but because drug rashes can escalate, many clinicians advise temporarily stopping HCTZ until the cause is determined. Decisions consider blood pressure control and alternative therapies.
How long does a hydrochlorothiazide rash typically take to resolve after stopping the drug?
Mild rashes often begin to improve within days and resolve in one to two weeks. More severe or drug-induced hypersensitivity reactions can take weeks to months to fully resolve, especially if systemic steroids or other treatments are required.
Can HCTZ cause photosensitivity and how can it be prevented?
Yes, hydrochlorothiazide can cause photosensitivity reactions: painful or itchy sun-exposed rashes. Prevention includes daily use of broad-spectrum sunscreen, sun-protective clothing, limiting peak sun exposure, and discussing alternative antihypertensives if recurrent photosensitivity occurs.
Are there tests to confirm an allergy to hydrochlorothiazide?
Specific tests are limited. Patch testing or delayed intradermal testing may help for certain reactions; oral challenge under specialist supervision is sometimes used if necessary. Blood tests for eosinophilia or liver/kidney involvement can support a diagnosis in systemic reactions. Consultation with an allergist/dermatologist is recommended.
If I have an HCTZ rash, are alternative blood pressure medications safe?
Many alternatives exist—ACE inhibitors, ARBs, calcium channel blockers, and other diuretics—but choice depends on your medical profile. Discuss alternatives with your clinician; they will weigh cross-reactivity risks, comorbidities, and blood pressure targets before switching.
How should adverse reactions to hydrochlorothiazide be reported?
In the U.S., report significant adverse reactions to the FDA MedWatch program online or by phone. Inform your prescribing clinician and, if hospitalized, ensure documentation in your medical record. Reporting helps safety monitoring and future prescribing guidance.
How can I reduce itch and skin irritation from an HCTZ rash at home?
Gentle skin care helps: cool compresses, fragrance-free moisturizers, oral antihistamines for itch, and avoiding hot showers or irritants. Use topical low-potency steroids for limited inflammation if advised by a clinician. Seek immediate care if signs of severe reaction appear.
When is emergency care needed for a hydrochlorothiazide rash?
Seek emergency care for acute facial or throat swelling, shortness of breath, high fever, blistering or peeling skin, mucosal involvement (eyes, mouth, genitals), or rapid spread—these signs suggest a severe systemic or life-threatening reaction.
How long after stopping HCTZ should I avoid re-exposure if I suspect a rash?
If you suspect HCTZ caused the rash, do not restart it until evaluated by your clinician or an allergist. In confirmed hypersensitivity or severe reactions, permanent avoidance is often recommended. Re-exposure can lead to more severe reactions.
Can skin biopsy determine if a rash is from hydrochlorothiazide?
A skin biopsy can show patterns consistent with drug-related hypersensitivity and help rule out other causes, but it is rarely diagnostic for a specific drug. Biopsy findings, clinical history, and timing together guide diagnosis.
How does an HCTZ rash differ from allergic contact dermatitis?
Allergic contact dermatitis is localized to where a substance touched the skin and evolves over days after contact; HCTZ rash is systemic and can be widely distributed, not limited to exposure sites. Photosensitivity rashes from HCTZ often affect sun-exposed areas but are drug-mediated.
How does HCTZ rash compare to urticaria (hives)?
Urticaria presents as transient, itchy wheals that fade within 24 hours and move around; drug-induced urticaria can be due to HCTZ. HCTZ-related rashes may be fixed maculopapular eruptions, photosensitive, or more persistent than classic hives.
How is HCTZ photosensitivity different from simple sunburn?
Photosensitivity reactions from HCTZ can produce exaggerated redness, blistering, or pigmentation changes after relatively brief sun exposure, often with itching. Sunburn is direct UV damage without drug involvement and generally correlates with intensity and duration of exposure.
How can you tell HCTZ-induced SJS/TEN apart from a severe drug eruption?
SJS/TEN features mucosal involvement (mouth, eyes, genitals), widespread epidermal detachment, target lesions, and systemic symptoms like fever—significantly more severe than typical drug eruptions. Rapid progression and blistering are key red flags requiring emergency care.
How does an HCTZ rash differ from DRESS syndrome?
DRESS (drug reaction with eosinophilia and systemic symptoms) includes a widespread rash plus fever, lymphadenopathy, eosinophilia, and organ involvement (liver, kidney). HCTZ can rarely trigger DRESS; look for systemic signs and lab abnormalities to distinguish it from isolated skin reactions.
How can you tell an HCTZ rash from a viral exanthem?
Viral rashes often occur with viral symptoms (fever, cough) and in epidemiologic settings; they can affect children and adults. Drug rashes often correlate with medication start or sun exposure and may improve after stopping the drug. Lab tests and history clarify the cause.
How does an HCTZ rash compare to chronic eczema (atopic dermatitis)?
Eczema is chronic, relapsing, typically associated with personal or family atopy and localized to flexures, with itching and lichenification. HCTZ rash tends to be acute, temporally linked to drug exposure, and often lacks the chronic distribution and history of atopy.
How is an HCTZ rash different from psoriasis?
Psoriasis causes well-demarcated, scaly plaques often on extensor surfaces and scalp, usually chronic with a genetic predisposition. Drug-induced rashes from HCTZ are typically more acute, less scaly, and linked to medication timing rather than the classic psoriatic plaque pattern.
Does an HCTZ rash look like a sulfa antibiotic allergy?
Both can present with maculopapular rashes, urticaria, or severe hypersensitivity. Because HCTZ contains a sulfonamide group, appearances can overlap; however, the pattern, timing, and severity vary. Discuss prior sulfa antibiotic reactions with your clinician when considering HCTZ.
How can you distinguish an HCTZ rash from contact dermatitis caused by a topical product?
Contact dermatitis usually appears only where the offending topical touched the skin and follows direct exposure. HCTZ rash is systemic and may appear on non-contact areas. A careful exposure history usually differentiates them.
How is an HCTZ rash different from heat rash (miliaria)?
Heat rash produces tiny sweat duct-blockage papules and prickly sensations in hot, humid conditions and resolves with cooling. HCTZ rash is medication-related, may be pruritic or painful, and often persists despite cooling until the drug is stopped.
How does an HCTZ-related photosensitive rash compare to cutaneous lupus erythematosus?
Both can worsen with sun exposure and affect sun-exposed areas, but cutaneous lupus often shows chronic, well-demarcated lesions with scarring or atrophy and may have autoimmune serology. HCTZ photosensitivity typically resolves after stopping the drug and avoiding sun.
